
On the flip side, to mitigate organizational exposure, they respond and execute containment plans when adverse and unforeseen situations transpire.ĭue to the dynamic and multifaceted nature of risk management in healthcare, the role is constantly evolving.
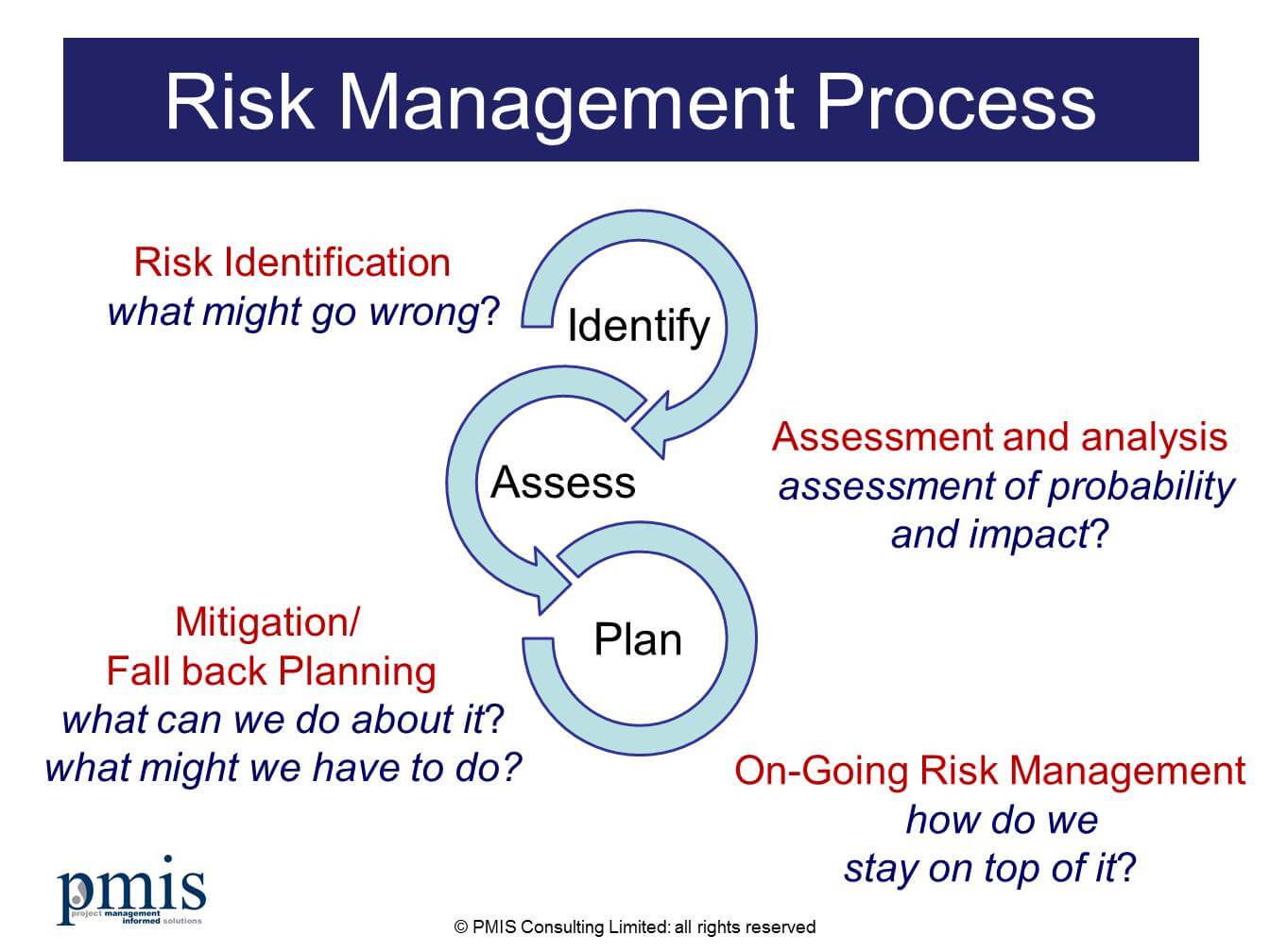
They also develop response plans incase risks become reality. Risk managers proactively identify risks and estimate potential consequences and upsides. The role of the healthcare risk manager has evolved alongside this new governance structure to oversee and facilitate the ERM framework. These elements of ERM are built on top of a governance structure that aligns business operations with the risk management program. Analytics are important for monitoring benchmarks as a way of showing value (what costs were prevented) for ERM initiatives.
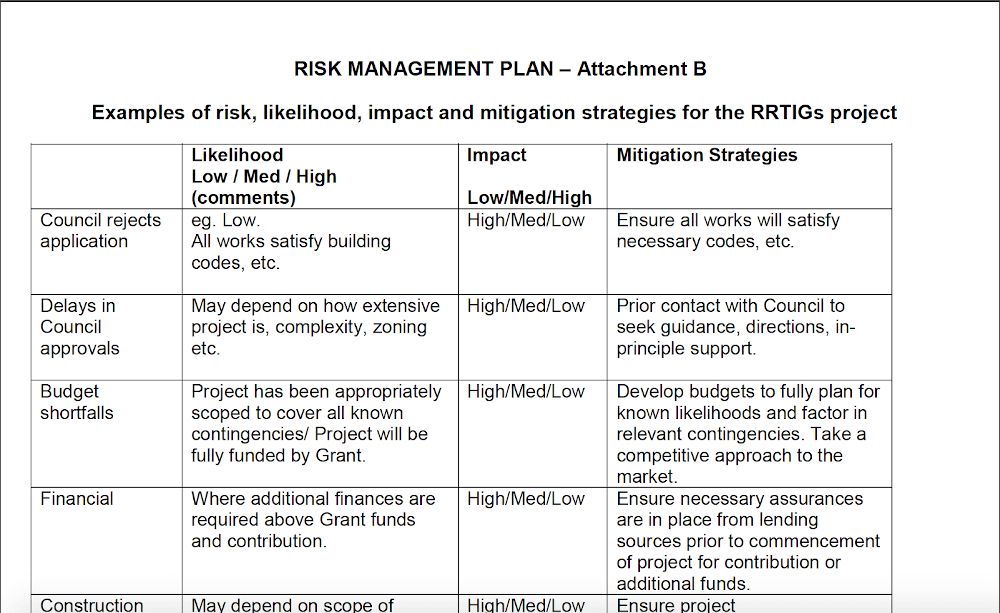
Additionally, data analytics are embedded to support decision-making, departmental cohesiveness, risk prioritization, and resource allocation. The current state for most providers falls between ‘basic’ and ‘evolving’ maturities for ERM programs.”Īccording to the American Society for Healthcare Risk Management ( ASHRM), “Enterprise risk management in healthcare promotes a comprehensive framework for making risk management decisions which maximize value protection and creation by managing risk and uncertainty and their connections to total value.”ĮRM also stresses the use of technology to synchronize risk mitigation efforts across the entire organization and remove risk associated with siloed departments or business units. According to the Healthcare Financial Management Association (HFMA), “Despite the growing importance of programs today, and the raised awareness of their importance, many healthcare providers have been slow to adopt a more sophisticated approach. While members of the industry understand the significance of expanding risk management in healthcare beyond patient safety and medical liability, the transition has been slow. In May of 2017, Moody’s Investor Services released a report highlighting the link between risk management and a hospital’s operating margins: “Maintaining high clinical quality will increasingly impact financial performance and reduce the risk of brand impairment as reimbursement moves away from a fee-for-service model and towards a greater emphasis on value and outcomes.”įor these reasons, hospitals and other healthcare systems are expanding their risk management programs from ones that are primarily reactive and promote patient safety and prevent legal exposure, to ones that are increasingly proactive and view risk through the much broader lens of the entire healthcare ecosystem.
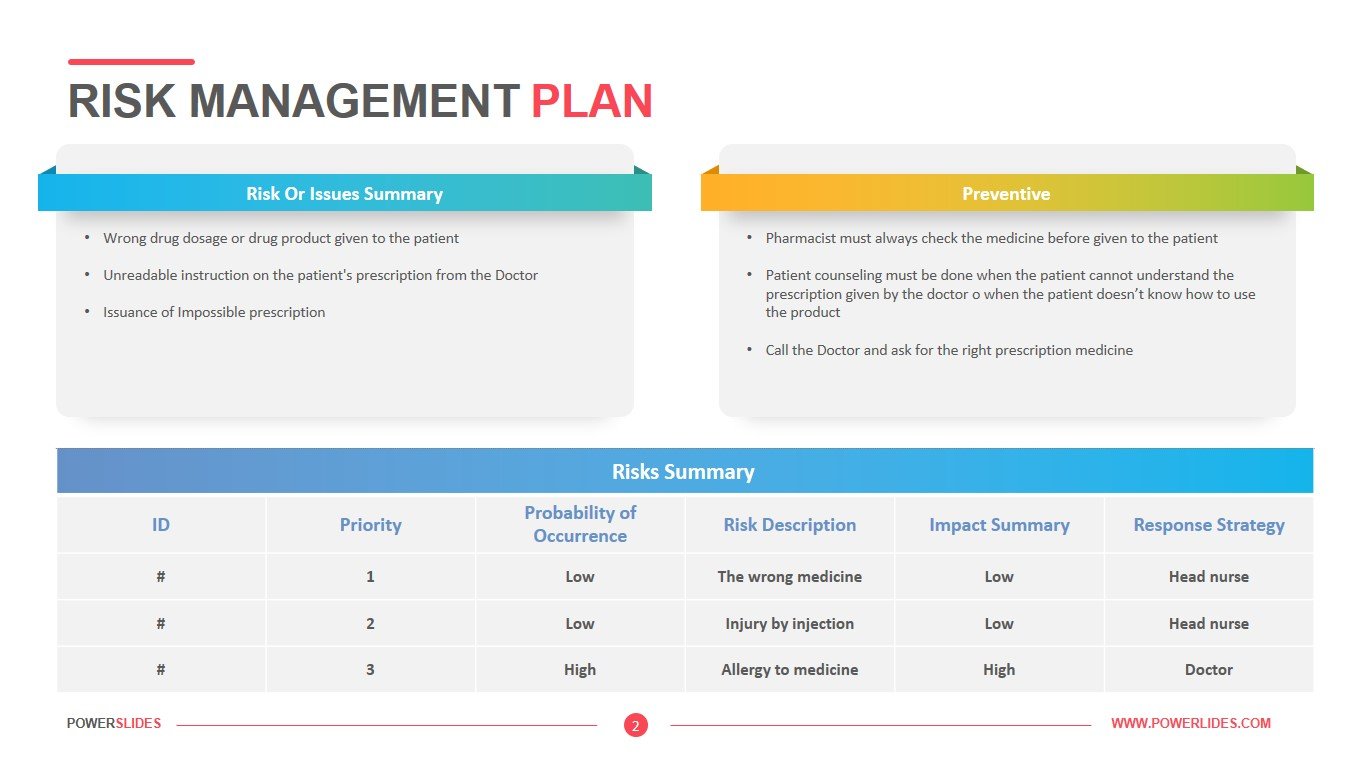
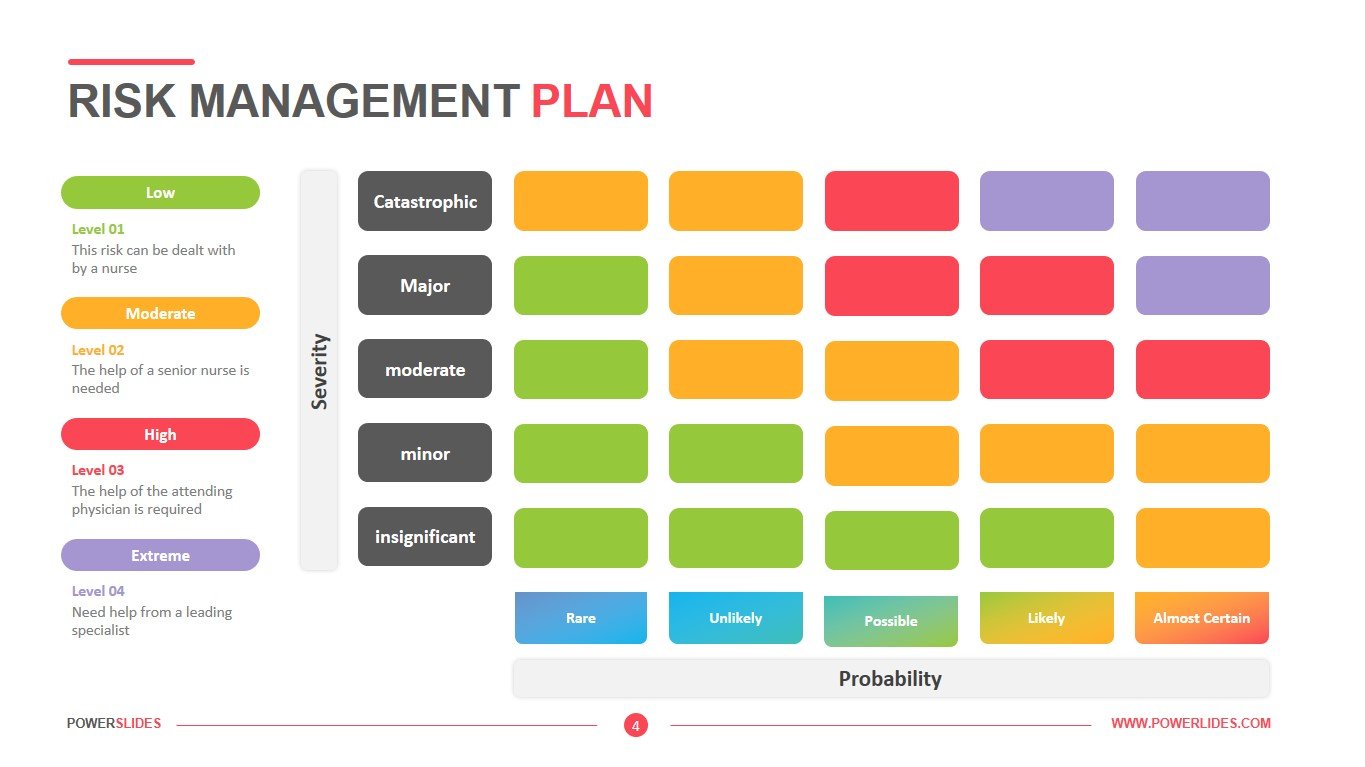

Moreover, with the value-based care movement and today’s risk-bearing models such as bundled payments and CMS’s pay for performance programs, financial risk is increasingly shifting from payers to providers and requires a broader view of risk management. But with the expanding role of healthcare technologies, increased cybersecurity concerns, the fast pace of medical science, and the industry’s ever-changing regulatory, legal, political, and reimbursement climate, healthcare risk management has become more complex over time. The Value and Purpose of Risk Management in Healthcare Organizationsĭeployment of healthcare risk management has traditionally focused on the important role of patient safety and the reduction of medical errors that jeopardize an organization’s ability to achieve its mission and protect against financial liability.

